Data Privacy in Healthcare: Smart Workflow Automation Strategies

Cheta Pandya

Patient data is one of the most valuable assets in healthcare today. In 2024, over 276 million U.S. patient records were breached, marking the highest exposure ever and fueling concerns about compliance and trust across the sector. Every record exposed isn’t just a number; it’s a person’s privacy at risk, an institution’s reputation on the line, and a compliance challenge waiting to happen.
As workloads increase and healthcare IT environments become more complex, protecting patient data demands a more innovative approach. Workflow automation in healthcare is key! By structuring and automating data handling, providers can minimize manual interventions, embed privacy safeguards, and lower overall risk while maintaining operational efficiency.
This is precisely why top hospitals are investing in advanced AI healthcare solutions to streamline workflows, secure data, and scale privacy protection with fewer errors.
Let’s explore actionable workflow automation strategies designed to help healthcare leaders safeguard patient information, maintain compliance, and keep their systems running smoothly.
What Is Data Privacy in Healthcare?
Data privacy in healthcare refers to the protection of sensitive patient information from unauthorized access, misuse, or disclosure. It is the practice of ensuring that protected health information (PHI) and personally identifiable information (PII) are collected, processed, stored, and shared in compliance with regulatory frameworks and ethical standards.
In healthcare, this practice goes beyond simple data protection. It establishes policies, technical safeguards, and access controls that prevent unauthorized disclosure, modification, or misuse of patient data.
This covers all forms of sensitive information, including electronic health records (EHRs), diagnostic reports, genetic data, insurance details, and treatment histories. The core objective is to maintain confidentiality, integrity, and availability (CIA triad) of healthcare data, ensuring it is accessed only by authorized entities for legitimate clinical or operational purposes.
Key Regulations That Shape Data Privacy in Healthcare:
- HIPAA (Health Insurance Portability and Accountability Act) in the U.S. sets national standards for protecting patient health information (PHI).
- GDPR (General Data Protection Regulation) in the EU applies strict rules on how healthcare providers store and share patient data.
- Local Regulations vary by country, but all share the same intent: safeguard patient privacy and enforce accountability in healthcare systems.
Why Data Privacy in Healthcare Demands Smarter Workflow Automation?
Healthcare is generating more data than ever before. From electronic health records (EHRs) and wearable devices to telemedicine platforms and AI-driven diagnostic tools, patient information is now spread across multiple systems and touchpoints. A major benefit is also observed in reducing hospital readmissions with AI. This explosion of data creates opportunities for better care, but it also raises serious privacy and security concerns.
Rising Cybersecurity Threats
In 2024, more than 725 data breaches were reported each day, exposing the protected health information (PHI) of 25,94,83,800 individuals. Attackers exploit system vulnerabilities, outdated IT infrastructure, and human errors to gain access. The result is costly breaches that not only disrupt care but also put patients at risk of identity theft and fraud.
Regulatory Pressure
Governments and regulatory bodies continue to tighten rules around the handling of protected health information (PHI). HIPAA 2025 security rule update mandates stricter safeguards and accountability to protect sensitive health information. Non-compliance is no longer an option—it can lead to severe penalties, audits, and reputational harm.
Digital Transformation in Care Delivery
With the rapid adoption of telehealth, mobile apps, and remote patient monitoring, data is moving outside traditional hospital walls. While these innovations improve accessibility and outcomes, they also expand the attack surface. Protecting patient data in these digital-first environments requires stronger security protocols and automated safeguards.
Patient Expectations
Patients today are more aware of privacy issues. They want to know how their data is being used, who has access, and whether their information is safe. Transparency and robust privacy measures are now essential for maintaining patient trust and ensuring active engagement in care.
What is Workflow Automation In Healthcare?
Workflow automation in healthcare means using technology to replace repetitive, manual tasks with digital processes that are efficient, consistent, and secure. It covers everything from patient admissions and appointment scheduling to billing, approvals, and medical record management, ensuring each step is executed seamlessly without unnecessary human intervention.
At its core, workflow automation in healthcare links electronic health records (EHRs), laboratory systems, scheduling apps, and compliance checks into a connected ecosystem digitizing how information moves, tasks are assigned, and decisions are made.
Automation not only streamlines paperwork and reduces errors but also cuts administrative workload, saves staff time, and improves patient outcomes by enabling more accurate, timely decisions. With HIPAA-compliant tools, it empowers providers to deliver safer, faster care, adapt to regulatory changes, and maintain seamless communication across clinical teams.
How Workflow Automation in Healthcare Works to Protect Data Privacy
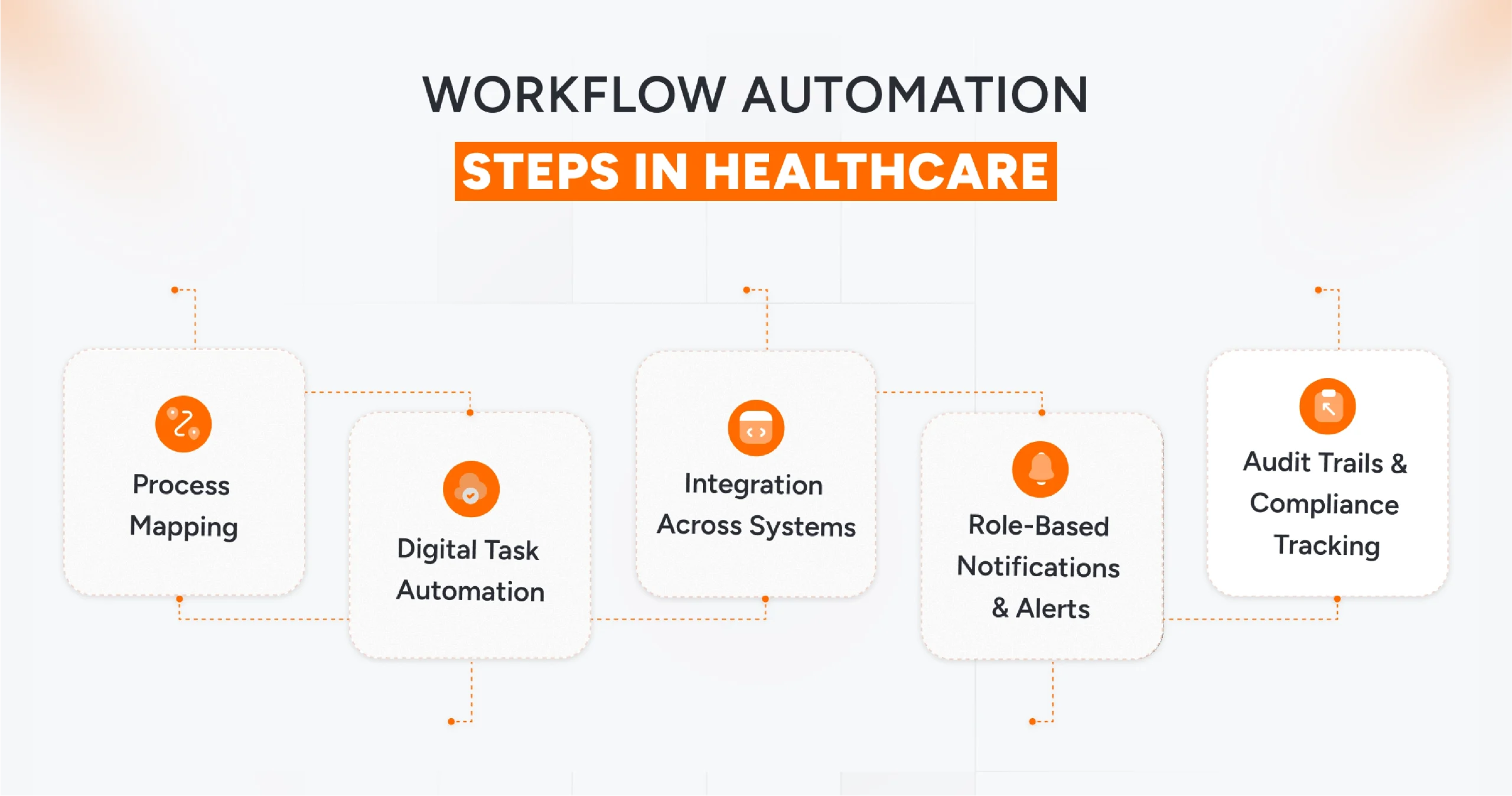
Healthcare systems today manage a range of processes, including patient intake, records management, billing, insurance verification, and clinical workflows.
Each of these involves sensitive patient data, manual touchpoints, and potential for error. Automation streamlines these processes while strengthening healthcare data privacy, compliance, and operational efficiency.
Process Mapping
- Identify and map existing workflows, including patient registration, lab reporting, and billing, while noting points where sensitive patient data is handled.
- Analyze steps for manual interventions or redundancies that could lead to unauthorized access or errors in PHI.
- Example: Mapping the patient intake process highlights where duplicate data entry or unencrypted storage could expose sensitive information.
Digital Task Automation
- Automate repetitive tasks to reduce manual handling of patient data.
- Examples include:
- Secure data entry into EHRs with validation checks.
- Encrypted appointment scheduling and reminders.
- Automated insurance verification and prior authorization, keeping sensitive financial and medical info protected.
- Generating reports for compliance or billing without exposing PHI in intermediate steps.
Integration Across Systems
- Connect disparate healthcare platforms, EHRs, lab systems, telehealth apps, and billing software to reduce manual transfers of PHI.
- Automation ensures secure, controlled, and auditable data flow between systems.
- Example: Lab results automatically update the patient’s EHR with encryption and access controls, reducing the risk of accidental exposure.
Role-Based Notifications & Alerts
- Send notifications only to authorized personnel based on their role, limiting unnecessary access to sensitive data.
- Example: A critical lab result triggers an alert to the doctor and a follow-up task for the nurse, without exposing PHI to non-authorized staff.
- This ensures privacy is maintained while care delivery remains timely.
Audit Trails & Compliance Tracking
- Log every automated action to create a comprehensive audit trail.
- Essential for regulatory compliance, including HIPAA and the HIPAA 2025 Security Rule Update
7 Strategies for Secure Workflow Automation in Healthcare
Healthcare organizations are under constant pressure to improve efficiency, cut down manual work, and provide better patient experiences. Workflow automation in healthcare helps achieve this, but privacy concerns can’t be ignored when dealing with Protected Health Information (PHI).
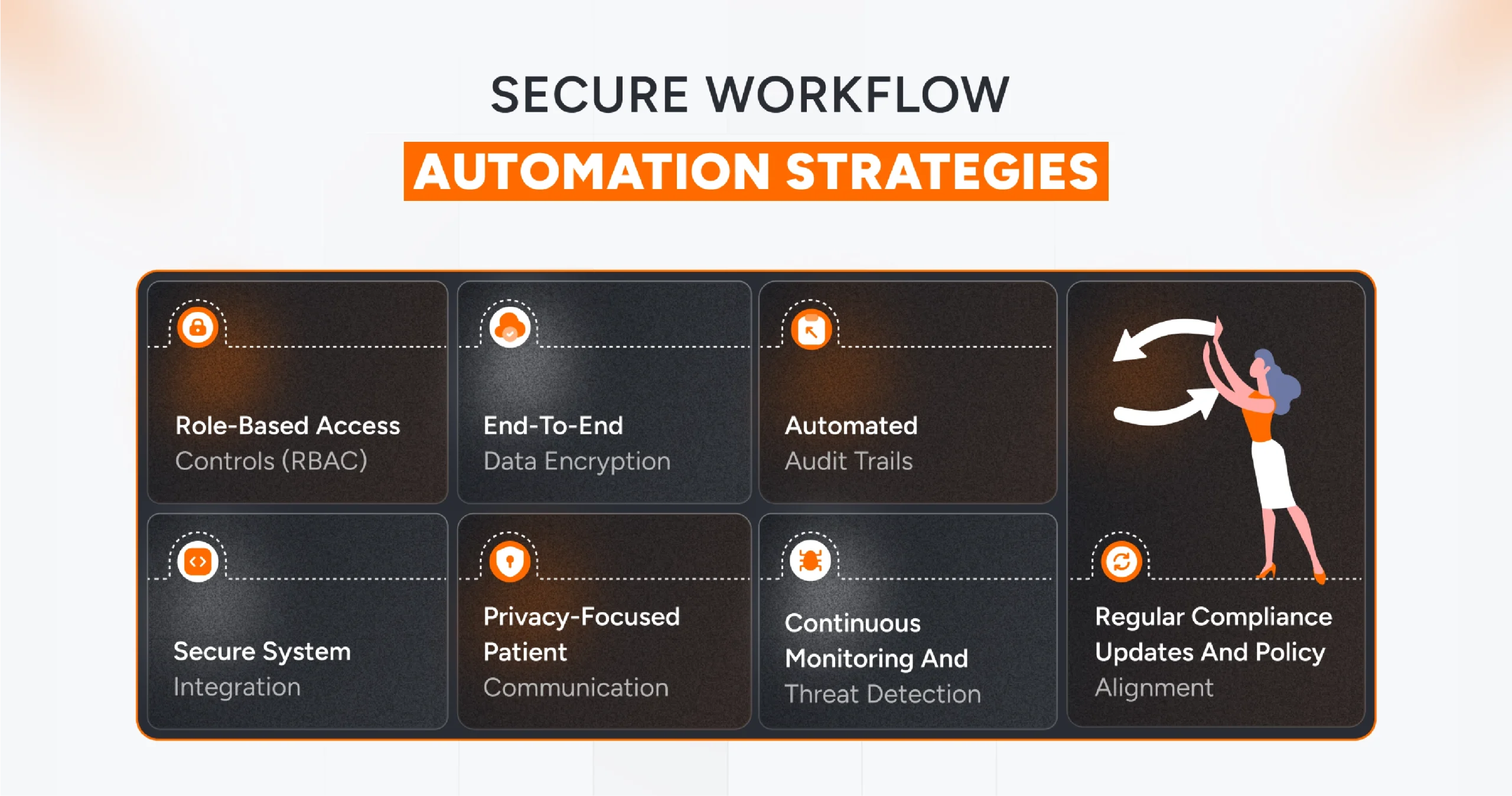
Below are detailed strategies that strike a balance between the benefits of automation and data privacy obligations.
1. Role-Based Access Controls (RBAC)
Access control is the first step to protecting patient records. In many hospitals, all staff may have broad access to information, which increases the risk of data misuse.
With RBAC, automation platforms assign permissions based on job roles. For example:
- Physicians access patient histories, prescriptions, and diagnostic reports to inform their treatment decisions.
- Nurses can view treatment plans and record vitals, but not billing data.
- Billing teams only access payment details, invoices, and insurance claims.
This structured approach ensures that staff see only what they need to perform their duties. It reduces the chance of insider threats and meets compliance requirements under HIPAA and GDPR.
2. End-to-End Data Encryption
Patient data is constantly moving—between EHR systems, diagnostic labs, and even external cloud platforms. Without encryption, these transfers can expose highly sensitive information. End-to-end encryption safeguards data:
- In transit: Lab reports, x-rays, or prescriptions sent electronically are protected while moving across networks.
- At rest: Data stored in hospital servers or cloud repositories stays encrypted, even if storage systems are compromised.
- Modern automation platforms also support tokenization (replacing sensitive data with tokens) for extra protection.
3. Automated Audit Trails
Every data access and update leaves behind a digital footprint. Audit trails generated by automation tools provide a clear record of all activity, including who accessed what, when, and why. This serves multiple purposes:
- Detects unusual behavior such as large-scale downloads by unauthorized users.
- Provides forensic evidence in case of a breach.
- Assures regulators that the organization follows best practices.
- Audit trails also build trust with patients, as they know their health records are monitored for misuse.
4. Secure System Integration
One of the most significant risks in healthcare is the integration gap between systems like EHRs, diagnostic labs, billing software, and insurance portals. Manual data entry or insecure APIs often create vulnerabilities.
Automation platforms with secure APIs and HL7/FHIR compliance allow seamless and safe data flow between systems. This reduces duplication, ensures data consistency, and eliminates the need for manual handovers that are prone to errors.
Insight for providers: Instead of layering multiple disconnected tools, adopting a centralized, secure automation solution prevents “data silos” and ensures consistent patient records.
5. Privacy-Focused Patient Communication
Automating communication improves patient engagement, but it’s also a common weak spot for data leaks. Sending sensitive health details over SMS or unencrypted emails can compromise privacy. Best practices include:
- Using secure patient portals or mobile apps for test results.
- Limiting text messages to ap pointment reminders only without medical details.
- Encrypting email notifications with password-protected attachments when needed.
6. Continuous Monitoring and Threat Detection
Automation should not stop at streamlining workflows. It must also actively monitor for potential threats in real-time. With AI-driven anomaly detection, healthcare organizations can catch unusual activities, such as:
- Multiple failed login attempts.
- Abnormal patterns in data transfers.
- Unauthorized system connections.
Proactive monitoring allows immediate response to threats before they escalate into full-scale breaches.
7. Regular Compliance Updates and Policy Alignment
Healthcare regulations, such as HIPAA, GDPR, and HITECH, evolve. Automated systems should be updated regularly to reflect these changes. Automation tools can help by:
- Sending compliance alerts when regulations change.
- Embedding updated consent policies into workflows.
- Maintaining up-to-date data handling protocols.
What are the Challenges of Healthcare Automation and Privacy?
Custom healthcare software development services promises faster workflows, fewer errors, and stronger patient engagement with automation. However, introducing automation also presents new challenges related to security, compliance, and trust. Providers who understand these challenges are better equipped to choose safe and effective solutions.
1. Managing Legacy Systems
Many hospitals still depend on legacy Electronic Health Record (EHR) systems that lack modern security features. Connecting these older platforms with new automation tools often creates weak points.
- Legacy databases may not support advanced encryption standards.
- Outdated APIs expose sensitive data during integrations.
- Manual workarounds to bridge gaps increase the risk of human error.
With modern innovations like AI-powered legacy electronic health record solutions, providers can enhance data interoperability, automate record management, and strengthen compliance without overhauling existing systems.
What providers should consider: When evaluating automation, check whether the platform supports secure integration protocols (HL7, FHIR, HIPAA-compliant APIs) that can work with existing systems without exposing PHI.
2. Balancing Speed and Security
Automation speeds up data transfers, scheduling, and reporting. But faster workflows can also mean faster mistakes if security isn’t embedded. For example:
- An AI assistant that schedules patient visits should not store unencrypted appointment histories.
- Automated billing systems must validate access requests before pulling financial records.
What providers should consider: Look for solutions that enforce role-based authentication and encryption at every step, even when processes are accelerated.
3. Ensuring Compliance with Evolving Regulations
Regulatory frameworks surrounding data privacy in healthcare are constantly evolving. HIPAA, GDPR, and the upcoming HIPAA 2025 Security Rule Update all require strict handling of PHI. Non-compliance leads to financial penalties and loss of trust.
- Automated systems must adapt quickly to new compliance requirements.
- Consent management should be integrated into workflows, rather than being handled separately.
- Audit trails should automatically update as policies evolve.
What providers should consider: Opt for automation solutions with built-in security and compliance solutions to ensure your workflows remain safe and up to date with industry standards.
4. Preventing Data Silos and Fragmentation
Automation often connects multiple departments—clinical, administrative, financial, and diagnostic. If these workflows are not centralized, data silos form. This makes it difficult to track information and exposes gaps where PHI can be misused.
- Patient data duplicated across unconnected systems creates inconsistencies.
- Fragmented workflows reduce visibility into who accessed sensitive records.
What providers should consider: Consolidated platforms with interoperability standards reduce fragmentation and create a single source of truth for patient data.
5. Addressing Human Factors
Even with advanced automation, human error remains a top cause of data breaches. Staff may mishandle automated alerts, ignore system warnings, or override privacy protocols.
A nurse might download patient files onto an unsecured device.
Administrative staff might use personal email to share automated reports.
What providers should consider: Automation must be paired with ongoing staff training and intuitive system design. The goal is to make secure behaviour the easiest behavior.
6. Monitoring Hidden Risks in AI Workflows
AI-driven assistants improve efficiency in scheduling, triage, and claims processing. But they also raise unique risks:
- Algorithms may access more patient data than required.
- Poorly configured AI workflows can expose PHI to third-party vendors.
- Lack of transparency in AI decision-making complicates compliance audits.
What providers should consider: Opt for AI workflow assistants in healthcare that provide explainability, data minimization, and strict auditability so PHI remains protected.
7. Preparing for Cybersecurity Threats
Healthcare is a top target for ransomware and phishing attacks. Automated workflows expand the attack surface, especially when multiple systems are connected. This is why the cost of a data breach has reached $4.4 million in 2025.
And what’s driving this increase,
- Hackers exploit misconfigured automation scripts.
- Unauthorized access attempts increase with the use of third-party integrations.
What providers should consider: Continuous monitoring, zero-trust frameworks, and real-time intrusion detection should be standard features of any automation platform.
Healthcare providers should choose digital transformation services with confidence when they focus on more than just speed. The ultimate goal is to implement safer processes that protect patient trust, comply with regulations, and maintain the organization’s strength.
How AQe Digital Helps Automate Your Healthcare Workflow?
Workflow automation in healthcare reduces administrative burdens, improves patient experiences, and allows providers to focus on care instead of paperwork. However, automation also raises serious concerns regarding data privacy in healthcare, compliance with evolving regulations, and the security of sensitive patient information.
At AQe Digital, we take a security-first approach to healthcare automation. Our solutions are built on robust encryption, strict access controls, detailed audit trails, and continuous monitoring. This ensures that while your workflows become more efficient, your data remains fully protected.
The result? A seamless balance between operational efficiency and patient data security, helping healthcare organizations scale with confidence. Contact us for a streamlined, secure, and efficient healthcare workflow automated through AI-based systems.


