How AI-Powered Legacy Electronic Health Record Modernization is Changing Healthcare Systems

Nirav Oza

Artificial Intelligence in the healthcare market is projected to grow from USD 20.9 billion in 2024 to an estimated USD 148.4 billion by 2029. However, even with this rapid growth cycle, many healthcare providers still continue to operate on their legacy information systems.
Such systems are expensive to maintain, expose providers to security risks, and slow efficient care. In an age when data security and systems reliability are critical, maintaining outdated technology exposes a fair arena for negligent conduct against patient safety and healthcare operations.
Failure to modernize legacy systems places an organization beyond simple inefficiency; in fact, this poses a clear danger to the security and operational stability of any organization. Legacy systems are becoming more vulnerable to cyberattacks and performance failures, exposing agencies and their clients to crippling risks.
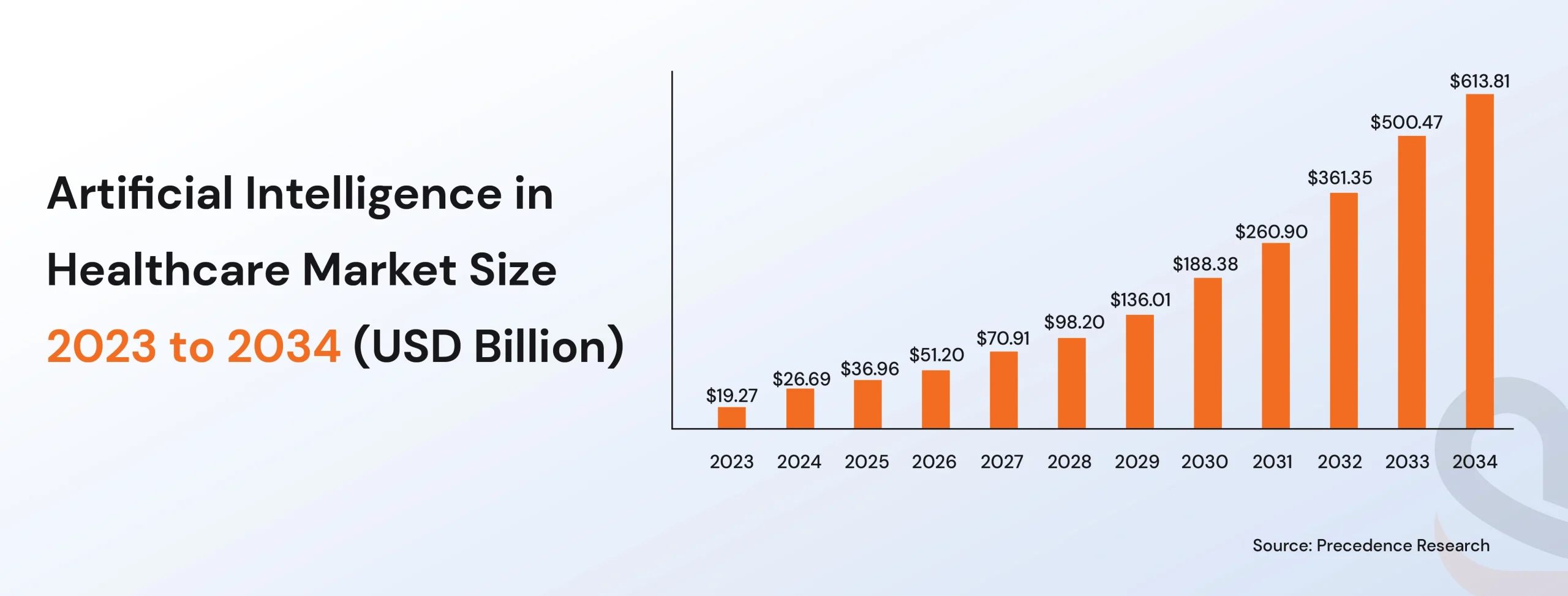
It’s clear that the cost of holding on to these antiquated systems is no longer sustainable. So, why are legacy systems failing healthcare providers, and what can be done to ensure that the future of healthcare isn’t left behind?
Why Legacy Systems Are Failing Healthcare Providers
Healthcare providers are expected to give the best of care on time, and the tools you rely on should help, not hinder, your ability to deliver excellent patient care. Let’s take a closer look at why AI-powered legacy EHR systems are becoming more of a liability than an asset:
Outdated Technology:
Legacy EHR systems were built on older infrastructure that really couldn’t meet the demands of the present. Mostly they work in silos, so new technologies are incompatible and severely limit the capability of your team to access and share patient data efficiently. These systems were built when healthcare practices were uncomplicated; however, they now struggle with maintaining cloud-driven data management, advanced analytics, and real-time integration. that modern healthcare demands.
Poor Interoperability:
Worst probably of all, the other significant downside of legacy EHRs is their poor interoperability. That says they can’t communicate well with each other or with other healthcare platforms of importance. This leaves patient data stored in separate silos scattered across providers, clinics, and hospitals. These create care gaps and treatment delays, increasing opportunities for error as clinicians grapple with incomplete or inconsistent data.
Very Costly to Maintain:
Maintaining outdated EHR systems is not just inefficient; it is also expensive. As the technology ages, support costs rise; specialized staff must be trained and retained to remedy the EHR system when it malfunctions. Because the vendor has gradually discontinued support for older versions of the software, healthcare organizations find it much more economically viable to make ad hoc fixes to these systems rather than replace them with a solution that would operate efficiently.
Limited Analytics and Decision Support:
Healthcare today is a lot about data-driven insight that helps inform clinical decisions. Most importantly, legacy EHR systems do not have capabilities for advanced analytics and AI-based decision support. Without this, healthcare is in a fragmented set of data with so little actionable insight, which ultimately compromises patient care and clinical outcomes.

Why AQe Digital Uses AI for Legacy EHR Modernization
Artificial Intelligence (AI) is no longer a futuristic concept; it’s already shaping how EHR systems operate, enhancing their capabilities, and driving efficiency. Here’s how AI is reshaping EHR systems and driving healthcare efficiency.
1. Advanced Data Integration and Interoperability
- Legacy EHR systems often work in silos, which makes sharing patient data from different sectors such as healthcare platforms and departments or even organizations nearly impossible thus stalling care to patients, creating. gaps in patients’ records and communications.
- The advanced interoperability standards today being adopted by advanced AI-EHR systems, like HL7 FHIR (Fast Healthcare Interoperability Resources), now allow seamless exchange of data across systems.
- The patient’s information could now be consistently updated and matched among systems as the AI algorithms could automatically map, clean, and normalize data obtained from different sources. The health care provider can thus always access live patient data for a faster and more correct decision.
- The advancements in interoperability would help link a whole chain of clinics, hospitals, pharmacies, and laboratories into a much better patient care coordination system of AI-powered EHR systems. Impact: Because of this, they would improve patient satisfaction and lower medical errors by enhancing care coordination and easing clinical processes.
2. Automation of Administrative Tasks
Automation is reducing administrative costs in healthcare by streamlining coding, billing, scheduling, and documentation, reducing errors and saving time.
For example, NLP could convert unstructured clinical notes into formally structured data for billing and coding, which not only makes billing and coding more accurate but also takes time away from clinical work. AI helps in:
- Automated coding and billing
- Documentation efficiency
- Intelligent scheduling
AI reduces the chances of coding errors and ensures reimbursement for health providers, improving revenue cycle management. AI algorithms automatically extract key clinical data from patient interactions, thereby not only reducing the time invested in manual charting but also allowing providers to spend more time with patients.
AI systems use predictive analytics to make optimal session scheduling considering patient history, capability of the clinic, and availability of provider personnel.
AI, by relieving the burden of administration, enables clinical staff to dedicate even more time to providing patient care while simultaneously reducing operational overhead and increasing financial performance.
3. Enhanced Clinical Decision-Support Systems
As health care in the modern world is fast-paced, doctors must make certain complex decisions immediately. Legacy EHR systems do not possess real-time clinical decision support (CDS) capabilities like the newer AI-powered EHR systems.
AI-based EHRs make use of machine learning and predictive analytics to analyze patient data (i.e., lab results, medical history, and symptoms) and come up with treatment, diagnosis, or preventive care recommendations based on evidence.
- AI algorithms train constantly from plenty of clinical datasets, recognize patterns, and flag possible risks, for instance, early signs of sepsis, drug interactions, or adverse events.
- Clinical decision support tools integrated with AI can alert the clinician in real-time of abnormal lab results, remind him of preventive screening, and provide guidelines for personalizing the treatment. Additionally, AI helps the clinician process large amounts of data that are too complex for human analysis alone, thus enhancing the accuracy of the diagnosis.
Fast and accurate decision-making results in improved patient outcomes, reduced misdiagnoses, and enhanced clinical efficiency for practitioners.
4. Strengthened Security with AI
Of course, old EHR systems have the major problem of cyber security in that these technologies are usually not as frequent at data breaches and cyberattacks. AI-powered EHR systems today incorporate security mechanisms that go beyond the usual encryption and access controls. Real-time threat detections, anomalies, and automatic responses by AI algorithms are used for protecting data from breaches.
- Continuous activity monitoring of the user behavior, its access to the system, and network traffic pours out information showing unusual occurrences that might reveal a possible cyberattack.
- AI can give presumptive knowledge and proactive mitigation of security weaknesses and can take automated actions like isolating suspicious activities or locking access to compromised systems.
- Moreover, data encryption, identification, and multi-factor authentication are all integrated into AI systems, protecting patient information from unauthorized access.
It protects patient privacy and organizational integrity, as AI in healthcare strengthens data security, lowers data breaches, and assists health organizations in conforming to compliant standards like HIPAA.
5. Predictive Analytics for Proactive Care Management
Predictive analytics allows AI-powered EHR systems to input historical data that could be retrievable for individual patients and generate outputs that will translate into actionable insights.
With predictive analytics applied to the machine learning algorithms in patient records, the AI system will capture the earliest signs of deteriorating health, for example, high risk for readmissions, infections, or complications.
- Predictive Models are those that will use patient demographics, medical history, and real-time clinical data to forecast possible outcomes, including hospital readmission or an onset of sepsis.
- AI could help providers prioritize high-risk patients when using resources efficiently. Most critical patients are closely monitored. Risk stratification powered by AI helps narrow down patients at risk of chronic disease progression so they can be intervened with earlier and given personalized care plans.
AI predictive analytics drive a sea change in patient outcomes by addressing the need for early intervention, decreasing readmission rates, and reducing expensive complications while optimizing resource utilization for the healthcare delivery system.
How AQe Digital Helps Healthcare Enterprises Modernize Legacy Systems for EHR
At AQe Digital, we believe in the evolution and the adoption of innovative solutions by healthcare enterprises. EHRs are doors that create boundaries, compromising operational effectiveness and patient care and creating vulnerabilities against security threats for a healthcare organization. Thus, based on our specialization, we focus on AI-powered EHR renovation that suits the peculiar requirements of care providers. Our approach helps you, as CIOs and tech leaders, overcome these barriers, enhancing system integration, security, and overall operational effectiveness to better support your organization’s evolving needs. Here’s why we insist on connecting with us:
- ⭐ Data Integration Expertise with AI – We renew legacy systems using AI for exchange and real-time updates of data.
- ⭐ AI Automating Administrative Tasks – We incorporate AI into legacy system environments to streamline coding, billing, and even scheduling.
- ⭐ AI-Assisted Clinical Decision Support – Enhancing legacy systems with real-time recommendations and better decision-making.
- ⭐ AI-Driven Security for Legacy Systems – Strengthening legacy systems with a security approach driven by AI and protected by real-time detection of threats.
- ⭐ Analytics Which Predict to Care Earlier – Using AI to feed its predictive analytics for identifying high-risk patients much earlier.
With AQe Digital knowledge and skills, one might realize the full potential of modernized EHR systems in enabling more efficient, secure, and patient-centered healthcare delivery by the organization.
